The recent publication of the Ontario experience in the introduction of Surgical Safety Checklists has caused a bit of a stooshie.
Checklists have consistently been shown to be associated with a reduction in death and complications following surgery. Since the publication of Atul Gawande’s seminal paper in 2009, checklists have been successfully introduced in a number of countries including Scotland. David Urbach and Nancy Baxter’s New England Journal of Medicine publication stands apart: the checklist made no difference.
Atul Gawande himself responded quickly asking two important questions. Firstly, were there sufficient patients included in the study to show a difference? Secondly, was the implementation robust and was the programme in place for long enough to expect a difference be seen.
He and others have reported the power of the study to be low – about 40% – meaning that were the study to be repeated multiple times and a true difference in mortality actually did exist, the chance of detecting it would be 40%. But power calculations performed after the event (post hoc) are completely meaningless – when no effect is seen in a study, the power is low by definition (mathsy explanation here).
There is no protocol provided with the Ontario study, so it is not clear if an estimate of the required sample size had been performed. Were it done, it may have gone something like this.
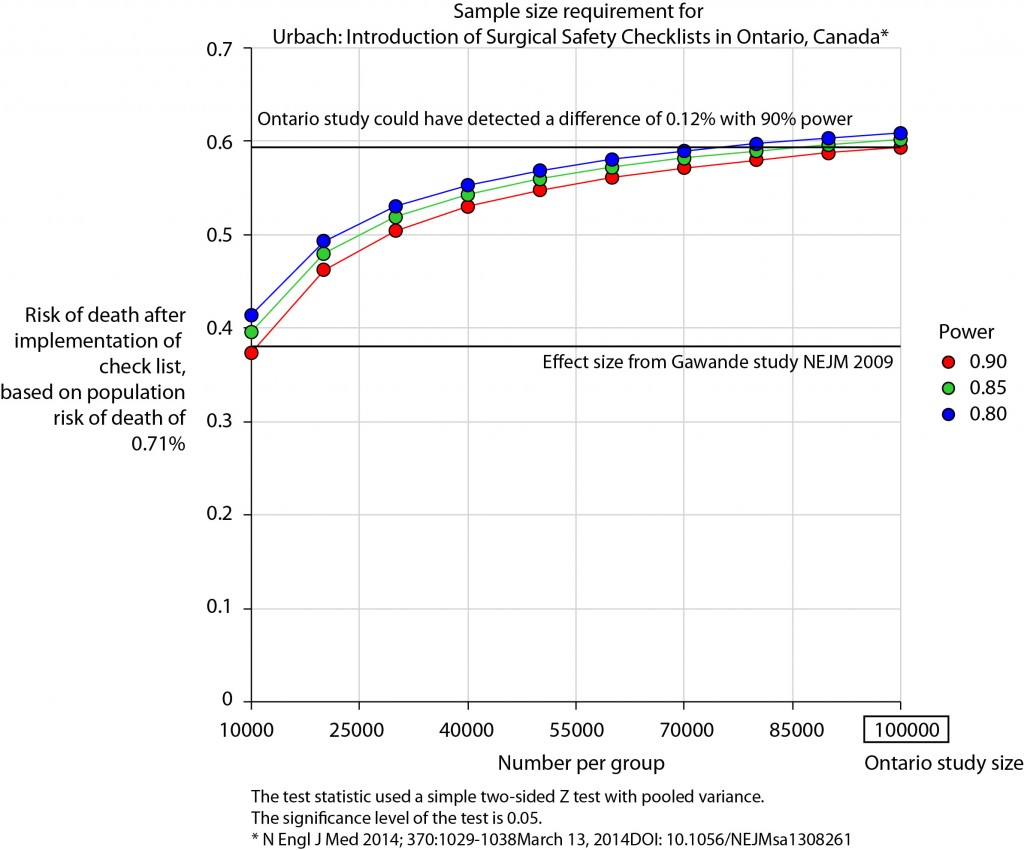
The risk of death in the Ontario population is 0.71%. This could have been determined from the same administrative dataset that the study used. Say we expect a similar reduction in death following checklist introduction as Gawande showed in 2009, 1.5% to 0.8%. For the Ontario population, this would be equivalent to an expected risk of death of 0.38%. This may or may not be reasonable. It is not clear that the “checklist effect” is the same across patients or procedures of different risks. Accepting this assumption for now, the study would have only required around 8000 patients per group to show a significant difference. The study actually included over 100000 patients per group. In fact, it was powered to show very small differences in the risk of death – a reduction of around 0.1% would probably have been detected.
Similar conclusions can be drawn for complication rate. Gawande showed a reduction from 11% to 7%, equivalent in Ontario to a reduction from 3.86% to 2.46%. The Ontario study was likely to show a reduction to 3.59% (at 90% power).
The explanation for the failure to show a difference does not lie in the numbers.
So assuming then that checklists do work, this negative result stems either from a failure of implementation – checklists were not being used or not being used properly – or a difference in the effect of checklists in this population. The former seems most likely. The authors report that …
… available data did not permit us to determine whether a checklist was used in a particular procedure, and we were unable to measure compliance with checklists at monthly intervals in our analysis. However, reported compliance with checklists is extraordinarily high …
Quality improvement interventions need sufficient time for introduction. In this study, only a minimum of 3 months was allowed which seems crazily short. Teams need to want to do it. In my own hospital there was a lot of grumbling (including from me) before acceptance. When I worked in the Netherlands, SURPASS was introduced. In this particular hospital it was delivered via the electronic patient record. A succession of electronic “baton passes” meant that a patient could not get to the operating theatre without a comprehensive series of checklists being completed. I like this use of technology to deliver safety. With robust implementation, training, and acceptance by staff, maybe the benefits of checklists will also be seen in Ontario.


Well done! An insightful analysis. It’s baffling that a study that is powered like this can be let down by inadequate follow-up time and simple methodological errors……hopefully they’re still collecting data and can reassess.
Agree. Suppose there are the same implementation difficulties in the UK.
Or, mayhaps there indeed *was* no effect. The Ontario study’s “starting” risk of death was less than half of the Gawande study’s…less, even, than the Gawande study’s ending risk of death. The Ontario study’s “starting” risk of complication almost half of the Gawande study’s ending risk of complication.
Maybe the Ontario hospitals’ surgical systems of care aer *better* than what can be achieved with a checklist…
Hi Wayne,
This is definitely possible, although I doubt it can be concluded from what we know at the moment.
The populations included in the two studies are not comparable. 20% of procedures in the Ontario series were for cataracts. The complication rate for these procedures is very low (0.79% in this large series). Unfortunately, the incidence of death and complications for subgroups is not included in the Ontario paper, so we do not know if the unadjusted outcomes are better in in Ontario (even not accounting for case mix).
But if the system failings that checklists are thought to mitigate against exist in Ontario, an effect would have been expected – even though the population risk is low. Checklists would not be expected to work less well on lower risk procedures, if the causes of poor performance are the same for high and low risk procedures.
So the lower complication rate appears to be explained by participant differences. But it may be that the bad stuff checklists help with doesn’t exist in Ontario. Do you think this is the case?
I don’t know, Ewen – I just pointed it out as a *possibility*…perhaps not likely, but still a possibility. 🙂
I admit to not reading the Ontario paper, only the synopses that hit the healthcare press. Your point about the different rates amongst the different subgroups of surgery types is a good one…